|
12/21/2023 0 Comments Right femoral neck fracture 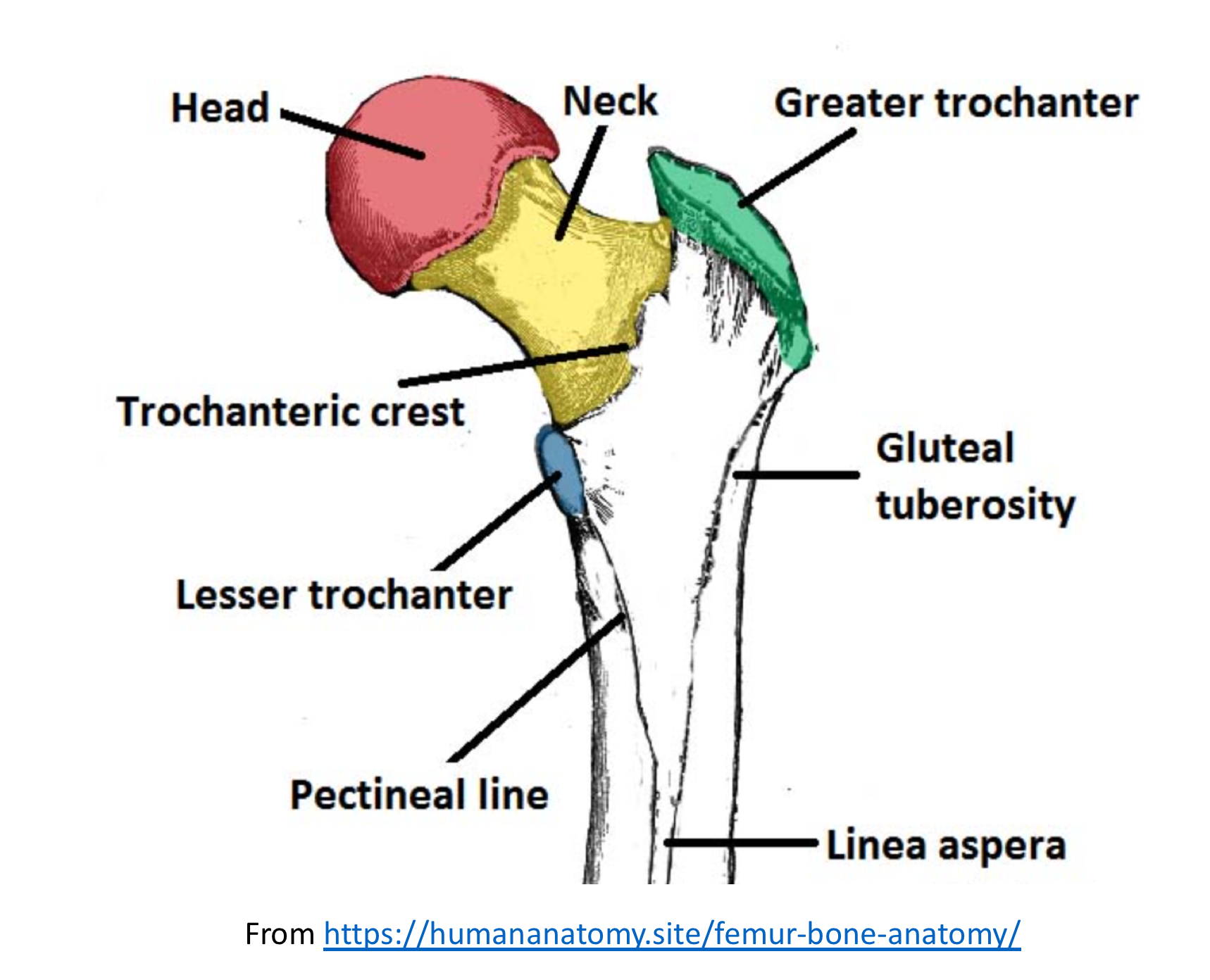
Weight-bearing status is determined by orthopedics. Treatment includes pain management, bed rest, and/or assisted mobilization.Some stable femoral neck fractures or simple avulsion fractures.Limited benefit of surgery (e.g., the patient has a terminal illness, severe dementia, and/or is nonambulatory).Extremely high perioperative risk (e.g., acute heart failure).Nonoperative management of hip fractures is uncommon as mortality rate is high. Įxpedite medical evaluation and perioperative optimization to facilitate an operative repair within 48 hours of admission. Program components include peripheral nerve blocks, avoidance of prolonged fasting, early removal of drains, and early ambulation.ERAS programs decrease the time to surgery, length of stay, and complication rate.Initiate an enhanced recovery after surgery program ( ERAS) if available at the local institution.Initiate weight-bearing activity immediately after surgery to decrease complications.Arthroplasty or hemiarthroplasty: displaced femoral neck fracture.Dynamic hip screw: nondisplaced base of femoral neck fracture.Cancellous screws: nondisplaced femoral neck fracture.Surgical technique depends on fracture location and characteristics.Timing: Ideally within 24–48 hours of admission.Operative intervention is recommended for most patients.See “ Trochanteric fracture” and “ Subtrochanteric fracture.”.See “ Femoral head fracture” and “ Femoral neck fracture.”.Treatment can vary depending on the fracture type and patient characteristics:.See also “ Hip fracture in older adults.”.Unexplained syncope: e.g., ECG, cardiac monitoring (See “ Syncope workup.”).Concurrent trauma: e.g., CT head (See “ Diagnostics in trauma.”).Additional preoperative testing for intermediate-risk surgery as indicatedĬonsider the following based on clinical presentation:.Suspect occult fracture despite normal x-rays in patients with characteristic clinical features of hip fracture. MRI hip and pelvis: preferred if an occult fracture is suspected.Evaluation for severe complications (e.g., clinical features of acute compartment syndrome, skin laceration suggestive of open fracture).Sciatic nerve injury (The sciatic nerve branches into the tibial nerve and common peroneal nerve.).Compare to the contralateral side if there is concern for arterial insufficiency.Assess femoral, popliteal, dorsalis pedis, and posterior tibial artery pulses.See “Subtypes and variants” for clinical features by fracture type. Perform the following prior to imaging of suspected hip fractures because they can impact acute management. Consult other specialists as needed (e.g., physical therapist, occupational therapist, nutritionist, social worker).Patients with hip fractures are often admitted to the hospitalist service or internal medicine.Anemia: Consider blood transfusion in symptomatic patients and/or those with hemoglobin 70 years of age are likely best treated in comprehensive geriatrics units (see “ Hip fracture in older adults”).See “ Hip fracture in older adults” for age-related comorbidities.  
The following conditions are commonly associated with hip fractures and should be managed early as they can impact perioperative outcomes. Avoid anticholinergics, muscle relaxants, benzodiazepines, and gabapentinoids because they increase the risk of delirium.Ī preoperative peripheral nerve block is recommended to improve pain control and reduce opioid consumption and the risk of perioperative delirium.Use NSAIDs with caution comorbid acute kidney injury ( AKI) is common.Use an opioid-sparing strategy (see “ Acute pain management” for details).Options: femoral block or fascia iliaca block by a trained specialist.Recommended for all patients without contraindications.Perform emergency preoperative assessment.Obtain bedside pelvis x-ray defer other hip imaging until the patient is stabilized.Unstable patients or those with polytrauma.Provide definitive hip fracture treatment based on fracture type (see “Subtypes and variants”).Admit to hospital and begin multidisciplinary care.Manage comorbidities that affect short-term outcomes (see "Acute management of comorbidities”).Obtain hip and pelvis x-rays and other hip fracture diagnostics as needed.Initiate multimodal pain management without delay (e.g., for confirmatory imaging).Identify associated injuries and complications that affect immediate management (e.g., open fracture, fracture-dislocation, neurovascular injury). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
